Infant Deaths Part 3 - Thrombocytopenia
Co-diagnoses, causes, complications and geographical distribution
Summary
Based on an analysis of proportion ratios of all diagnostic-keys mentioned in infant deaths between the years 2015 and 2022, the year 2022 stands out as highly unusual with a total of 55 diagnostic keys representing significant (p<0.001) safety signals, compared to a maximum of 11 safety signals in the preceding years.
One of the most striking signals is neonatal thrombocytopenia, with a 2022 proportion ratio of 12.9 (99.9% CI: 6.0-27.5) compared to the previous 7 years.
Further analysis revealed that the most common causes for the 68 neonatal deaths involving thrombocytopenia were intrauterine hypoxia and bacterial sepsis.
Furthermore, 29 cases resulted in intraventricular haemorrhage (bleeding into the intraventricular space of the brain), which likely represents the mechanism resulting in the deaths of these 29 infants. Intraventricular haemorrhage itself is an important 2022 safety signal that we isolated in the previous article of this series, involved in at least 80 excess infant deaths.
Almost a quarter (23.5%) of the 68 thrombocytopenia deaths occurred in Florida and Mississippi, which make up only 7.5% of the national population. These states were heavily vaccinated amidst the summer catastrophe of 2021, when Mississippi saw by far the largest number of fetal deaths per live birth.
Introduction / Recap
In part 1 of this series we identified a troubling signal in U.S. infant mortality, but trend-correction was neccessary to spot it and we weren’t able to explain the signal through maternal or infant COVID vaccinations.
In part 2 we got an overview of diagnoses by MCOD (Multiple Causes Of Death) that saw unusual increases in 2022.
Today I am going to do two things:
Look at the number of signals for all years between 2015 and 2022 to illustrate how unusual the year 2022 is in terms of changes in the distribution of infant mortality causes.
Take a closer look at the P61.0 signal (transient neonatal thrombocytopenia).
Which other diagnostic keys are commonly found on death certificates of infants whose death involved a diagnosis thrombocytopenia?
In which regions did these deaths occur?
Methods
I used CDC Wonder to download annual infant deaths occurring in the years 2015 through 2022, both by UCOD (Underlying Cause Of Death) and MCOD (Multiple Causes Of Death). Data for these 8 years was available for…
394 causes of death by UCOD
713 causes of death by MCOD
To identify signals I chose proportion ratios:
Count the total number of infant deaths occurring throughout…
…the year in question (n1)
…the remaining 7 years (n2)
Count the number of deaths with the respective diagnostic key throughout…
…the year in question (x1)
…the remaining 7 years (x2)
With these 4 figures I can calculate proportion ratios. The formula is:
pr = (x1/n1) / (x2/n2)
Since we are doing this for a total of 713 signals, we should expect a lot of false positives. To minimize the number of these false signals, I am calculating 99.9% confidence intervals for each diagnostic key.
Only keys which ratio is significantly (p<0.001) higher or lower than 1 generate a signal.
Results
First we take a look at the annual number of signals.
Negative signals (blue) are diagnostic keys that are mentioned in a significantly lower proportion of infant deaths than throughout the other 7 years. They range between 0 and 13 signals per year throughout the entire 8 years.
Positive signals (red) are actual safety signals - keys that are mentioned in a significantly higher proportion of infant deaths in the respective year compared to the other 7 years. They range between 0 and 11 from 2015 through 2021.
In 2022, the number of signals rises to 55. That’s five times as many safety signals as in 2021 or any other year since 2015.
This in itself is a very strong safety signal, that warrants immediate investigation by U.S. government authorities.
Sometimes changes to how deaths are coded can cause some diagnostic keys to be used more or less frequently than during previous years. This could be the case for some, but surely not all of these 55 signals.
There’s something happening - that’s for sure. The reason I showed you the chart is to make that crystal clear!
The strongest of these signals is transient neonatal thrombocytopenia (ICD-10 code P61.0), with a 2022 proportion ratio of 12.9 (99.9% CI: 6.0-27.5). That means it was mentioned on almost 13 times as many death certificates compared to the 7 years preceding 2022.
Transient neonatal thrombocytopenia (P61.0)
While thrombocytopenia (low platelet count) is a common occurrence in neonates, it rarely causes death. To give you an idea how unusual this cluster of deaths is, I’ve downloaded monthly data from 2018 through 2023.
There were 18 infant deaths in which thrombocytopenia was mentioned on the death certificate between 2018 and 2021. By the end of the first quarter of 2023 this number increased to 86.
While there is only a single diagnostic key coding for the problem, there is a large array of etiologies that can lead to neonatal thrombocytopenia. Some of these are more common when the problem occurs in the fetus, some are more commonly responsible in the first few days after birth (<72h), others are more likely to be responsible when the onset happens later (>72h).
Causes of transient neonatal thrombocytopenia
Fetal thrombocytopenia
Alloimmune: NAIT (neonatal alloimmune thrombocytopenia) occurs when maternal antibodies are attacking paternal platelets and usually presents as a severe platelet deficiency
Autoimmune (maternal autoantibodies, in many cases due to the mother having idiopathic thrombocytopenic purpura or systemic lupus erythematosus)
Congenital infection (most often viral, e.g. cytolomegavirus, toxoplasma, rubella)
Chromosomal disorders (mostly trisomies or triploidies)
Early-onset thrombocytopenia (<72h)
Alloimmune: NAIT (see fetal thrombocytopenia)
Autoimmune (see fetal thrombocytopenia)
Chronic intrauterine hypoxia, placental insufficiency (e.g. due to pre-eclampsia or diabetes)
Perinatal asphyxia
Disseminated intravascular coagulation (DIC)
Necrotizing enterocolitis (NEC)
Occult infection
Late-onset thrombocytopenia (>72h)
Sepsis
Necrotizing enterocolitis (NEC)
A closer look at co-diagnoses
Since decedent-level data (death certificates) are not publically available and more detailed infant death data including information about the newborns are only available for 2021, I queried CDC Wonder to find out which other diagnostic keys were present in the 2022-2023 cluser of 68 infant deaths, where thrombocytopenia was mentioned on the death certificate.
Causes
In 20 cases the cause was likely intrauterine hypoxia
In 6-9 cases the newborn developed necrotizing enterocolitis, which can be a cause for thrombocytopenia in the newborn
In 23 cases the newborn developed sepsis. In two more instances other perinatal infections were likely the cause.
Some other P-codes (perinatal) and Q-codes (congenital abnormalities) might have caused the problem to manifest, but we lack more detailed data on these codes
Indirectly linked
Both hypotension and renal failure are relatively common in sepsis.
It is unclear whether or not there is a direct causal link between hypotension and renal failure, but they often co-occur
Complications
Thrombocytopenia explains 29 of the roughly 80 excess P52 deaths (Intraventricular nontraumatic haemorrhage of newborn). This is bleeding into the intraventricular space of the brain.
So it seems the most common causes are intrauterine hypoxia and bacterial sepsis. While this alone won’t explain what is going on it helps to know that there isn’t just a single cause for these excess infant deaths involving thrombocytopenia.
What’s more important is, that we’ve identified the cause of 29 excess neonatal deaths involving intraventricular haemorrhage - a large significant (p<0.001) signal first isolated in the last part of this series.
Let’s have a look at where these deaths occurred.
Geographical distribution
First, a simple list of…
all infant deaths 2022-2023
infant deaths involving thrombocytopenia
the proportion of the latter among the former
…by maternal state of residence.
The cluster of thrombocytopenia deaths did not occur in just a single state, suggesting a systemic problem.
However, what is very striking: Over 23% of the 68 thrombocytopenia deaths occurred in Florida and Mississippi, which make up less than 8% of the national population. These states were heavily vaccinated in Q3 2021, when Mississippi saw by far the largest number of fetal deaths per live birth.
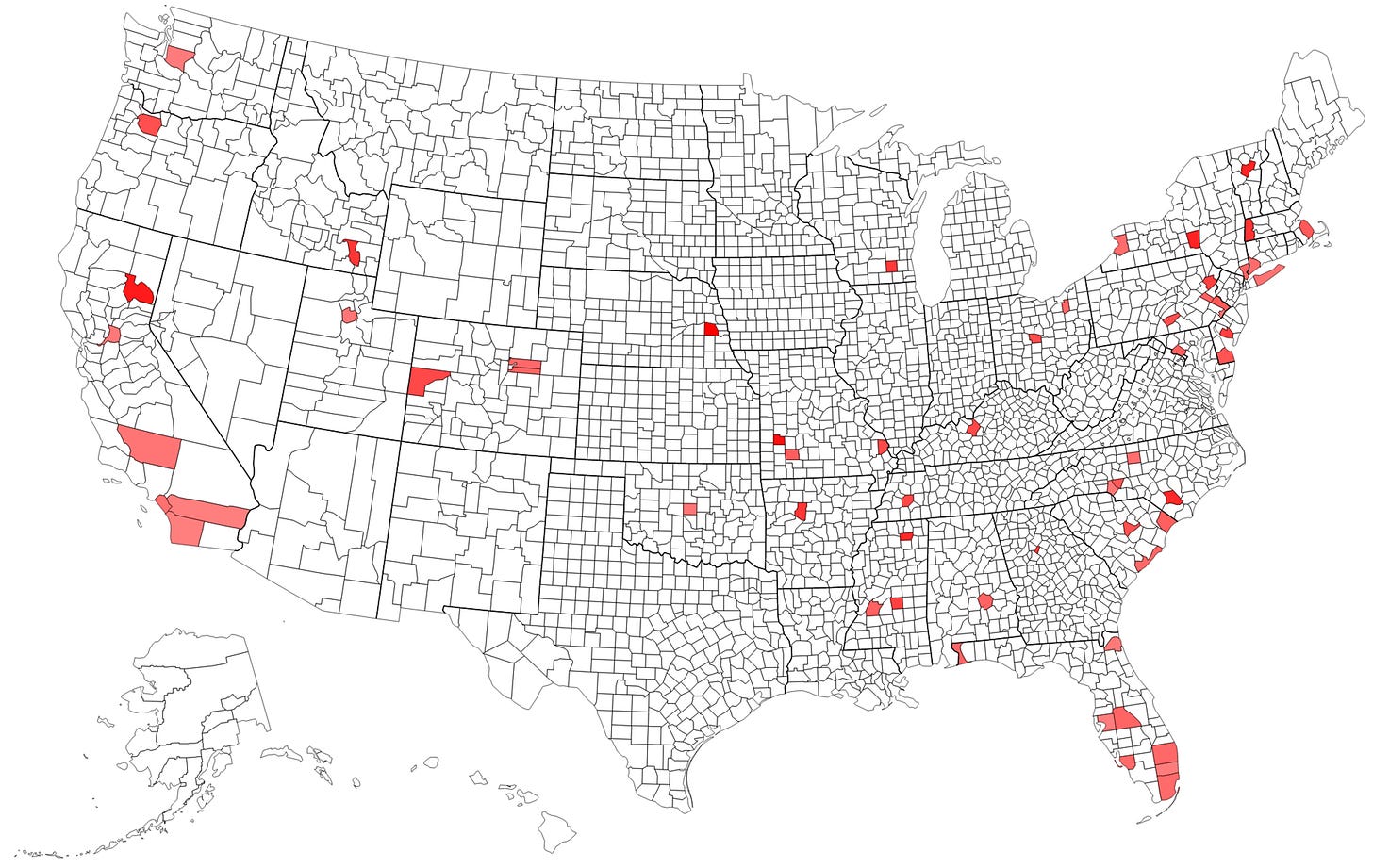
Here is a look at the counties that registered these deaths.
Darker colors represent higher proportions among all infant deaths.
Counties with more than 1 neonatal thrombocytopenia death in Florida:
4 deaths in Miami-Dade County
2 deaths in Palm Beach County
2 deaths in Polk County
Counties with exactly 2 neonatal thrombocytopenia deaths (other states):
Orange County, CA
Montgomery County, MD
Philadelphia County, PA
The other 54 thrombocytopenia infant deaths were single occurrences across the remaining counties.
VAERS signal
I run a website called pervaers.com which lists safety signals generated from the publically available VAERS database. Signals for thrombocytopenia have been present in all age groups for some time now, but are rarely talked about.
These are proportional differences (along with 90% confidence intervals) between the proportion of U.S. Pfizer adverse event reports mentioning “immune thrombocytopenia”, relative to a age- and gender-adjusted pseudo-placebo report cohort. If you want to learn more about how the reference cohort is generated, you can find this information in the help section of pervaers.com.
The signal is present for Moderna as well, but not in the lowest age tiers, due to the low number of Moderna doses administered to children.








Fabian what a monumental effort. A mission one would suspect would be a core purpose of any public health agency but deliberately ignored. Thanks for looking out for us. This data will help us ignore future corrupted mandates from these maniacal agencies and maybe with luck be used to hold those most responsible for the deaths they caused to some form of accountability.
Yet another hard hitting analyses. This is armor-piercing material. Sadly, the FDA et al. seem to have upped their bullet-proofing lately. But the bar chart carries heavy messaging to the people 💪
Speaking as a father of three:
The horror of the fates behind the numbers is spine-chilling.